Table of Contents
Types Of Hip Replacement Surgery
Use this checklist of questions to guide your decision-making: Are you certified by the American Board of Plastic Surgery? How many years of plastic surgery training do you have? How long have you been performing breast lift surgery? How many breast lift surgeries do you do a year? Do you have hospital privileges to perform breast lift surgery? If so, where? Is your office surgical facility accredited by a nationally- or state-recognized accrediting agency, or is it state-licensed or Medicare-certified? Am I a good candidate for a breast lift? Should I wait until after pregnancy to have a breast lift? Should I combine a breast lift with breast augmentation surgery? What surgical technique is recommended for me? How long will the operation take? Which incision technique would be most effective in my case? Will I have general anesthesia, and will a certified anesthesiologist administer it? Where and how will you perform the procedure? What are the risks and complications with this procedure? How long of a recovery period can I expect, including time away from work? What kind of help will I need during my recovery? What can I do to lower the risk of short-term and long-term complications? Where will my scar be? Can I see some patient before-and-after photos? What are my options if I am dissatisfied with the outcome of the surgery? How much pain or scarring will I experience following surgery? What can I expect my breasts to look like over time? How can I expect to look after pregnancy? Will a breast lift affect my ability to breastfeed in the future? How long can I expect results to last? What kind of additional follow-up will I need? Because breast reduction surgery is tailored to each woman's individual needs, having an honest discussion with the breast surgeon about the procedure will help you to understand what is involved and what to expect.
The amount depends on the location, surgeon, type of procedure and type of implant (if used), as well as fees for anesthesia, surgical facility costs and postoperative medications. Typically, health insurance does not cover cosmetic procedures, like breast augmentation, but health plans will cover surgeries that are considered "medically necessary," such as breast reconstruction and some breast reductions.
Research shows that those who are empowered: Do online research Ask a lot of questions Are in contact with other patients Access and review their own health data (like electronic health records) Applying these actions to decisions about breast surgery and being proactive and ready to ask questions leads to having defined goals and realistic expectations, better interactions with the surgical team and a better chance of satisfaction with the surgical outcome.
Total Hip Replacement Surgery Technique
e. the breast itself), surgeons have more control over bleeding and precision than they do with other incisions, like the transaxillary or umbilical incision. It allows for excellent access and vision of the pocket to achieve accurate and optimal placement of the implant. The original incision site can be reopened for subsequent surgeries, if necessary.
For example, if a woman decides to increase her breast size, this might make the scar move up so it is on the breast itself. On the other hand, if she decreases it, the scar can move down so it is visible below the fold of the breast. For patients who undergo breast augmentation with very small breasts to begin with or have no natural breast crease, it is sometimes difficult for a plastic surgeon to place the incision in an optimal position.
Advantages of the Periareolar Incision: The scar often heals well compared to other breast augmentation incisions. If the incision is delicately placed at the precise junction of the dark areolar skin and the lighter colored surrounding skin, the scar is barely noticeable. Sometimes, a periareolar incision is camouflaged so well it is nearly invisible.
How Do They Do Hip Replacement Surgery

Similar to inframammary incisions, a periareolar incision point can be reopened and reused if future surgeries on the breast are needed. Disadvantages of the Periareolar Incision: Of all the breast augmentation incisions, the periareolar incision is associated with the greatest chance of inability to nurse a child after the procedure, although the risk is quite low.
In some cases, this may require corrective surgery. There is also a slight increase in the risk of altered nipple sensation compared with the other incisions. Some studies have suggested that a periareolar incision poses a higher risk of capsular contracture than do the other incision types. The periareolar incision should only be used when the areola has sufficient diameter to allow for insertion of an implant.
Considering there are no incisions on the breast, wearing any kind of bathing suit, undergarments, and low-cut tops without worrying about a visible scar is easily accomplished. Disadvantages of the Transaxillary Incision: It can be difficult to position the breast implant in the popular “dual plane location”, which many plastic surgeons believe is the optimal position for implants in most patients.
Hip Joint Ball Replacement Surgery
The TUBA incision often leaves an undetectable scar, as it is hidden within the wrinkles of your naval. The recovery time is typically shorter compared to other breast incision types. Disadvantages of the Trans-Umbilical Breast Augmentation (TUBA) Incision: The TUBA scar, in most cases, cannot be reopened. This means additional incisions are needed if problems arise with the placement of your implants and your doctor has to perform revision surgery, or if you decide to go up in size or have a breast lift later.

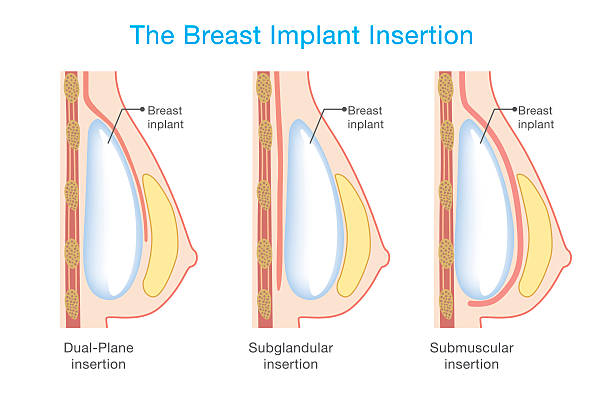
Sometimes, this capsule becomes thickened and larger. This may cause a change in the shape of your breast, hardening of breast tissue, or some pain. Emotional risks for this surgery may include feeling that your breasts do not look perfect. Or, you may be disappointed with people's reactions to your "new" breasts.
Navigation
Latest Posts
Do I Need Hip Replacement Surgery
Latest In Hip Replacement Surgery
Hip Replacement Repair Surgery